Millions of people in the United States are currently living with limb loss. This number is expected to grow as the population ages and rates of diseases such as diabetes that can cause dysvascularity (poor blood circulation in the legs) increase.
For people with limb loss, prosthetic devices improve quality of life by providing movement and independence. Early prosthetics were uncomfortable to wear, but they may have helped people return to work and feel accepted in their daily lives. We’ll explore how these devices have changed over time, from clunky, early designs and materials to modern innovations—some of which NIH-supported researchers are developing.
When were prosthetics invented, and what were they used for?
Historians don’t know for certain if the first prosthetics were functional or for appearances. According to Katherine Ott, Ph.D., curator for the Division of Medicine and Science at the Smithsonian Institution’s National Museum of American History, this is partly because different cultures have their own ideas about what makes a person whole.
The oldest known prosthetics are two different artificial toes from ancient Egypt. One prosthetic toe, known as the “Greville Chester toe,” was made from cartonnage, which is a kind of papier-mâché made from glue, linen, and plaster. It is thought to be between 2,600 and 3,400 years old, though its exact age is unknown. Because it doesn’t bend, researchers believe it was cosmetic.
The other prosthetic, a wooden and leather toe known as the “Cairo toe,” is estimated to be between 2,700 and 3,000 years old. It is thought to be the earliest known practical artificial limb due to its flexibility and because it was refitted for the wearer multiple times.
Approximately 300 years later—300 B.C.—in Italy, an ancient Roman nobleman used a prosthetic leg known as the “Capua leg.” The leg was made of bronze and hollowed-out wood and was held up with leather straps.
Other known early prosthetics include artificial feet from Switzerland and Germany, crafted between the 5th and 8th centuries. These were made from wood, iron, or bronze and may have been strapped to the amputee’s remaining limb.

A wood and aluminum prosthetic arm invented by William Robert Grossmith in the mid-19th century.
How war—and the U.S. military—inspired prosthetic advances
Soldiers who lost their limbs in battle often used early artificial limbs made of wood or iron. For example, about 2,200 years ago, the Roman general Marcus Sergius Silus lost his right hand during the Second Punic War. He had it replaced with an iron one that was designed to hold his shield. Knights of the Middle Ages sometimes used wooden limbs for battle or to ride a horse. And in the 16th century, the French surgeon Ambroise Paré designed some of the first purely functional prosthetics for soldiers coming off the battlefield. He also published the earliest written reference to prosthetics.
Then came the American Civil War in 1860. The record number of amputees from the war caused the number of patents for prosthetics to almost quadruple. One of these patents was for a wooden leg called the “Hanger limb.” It was the first to use rubber in the ankle and cushioning in the heel, showing that inventors understood they needed to make prosthetics less painful for amputees to wear.
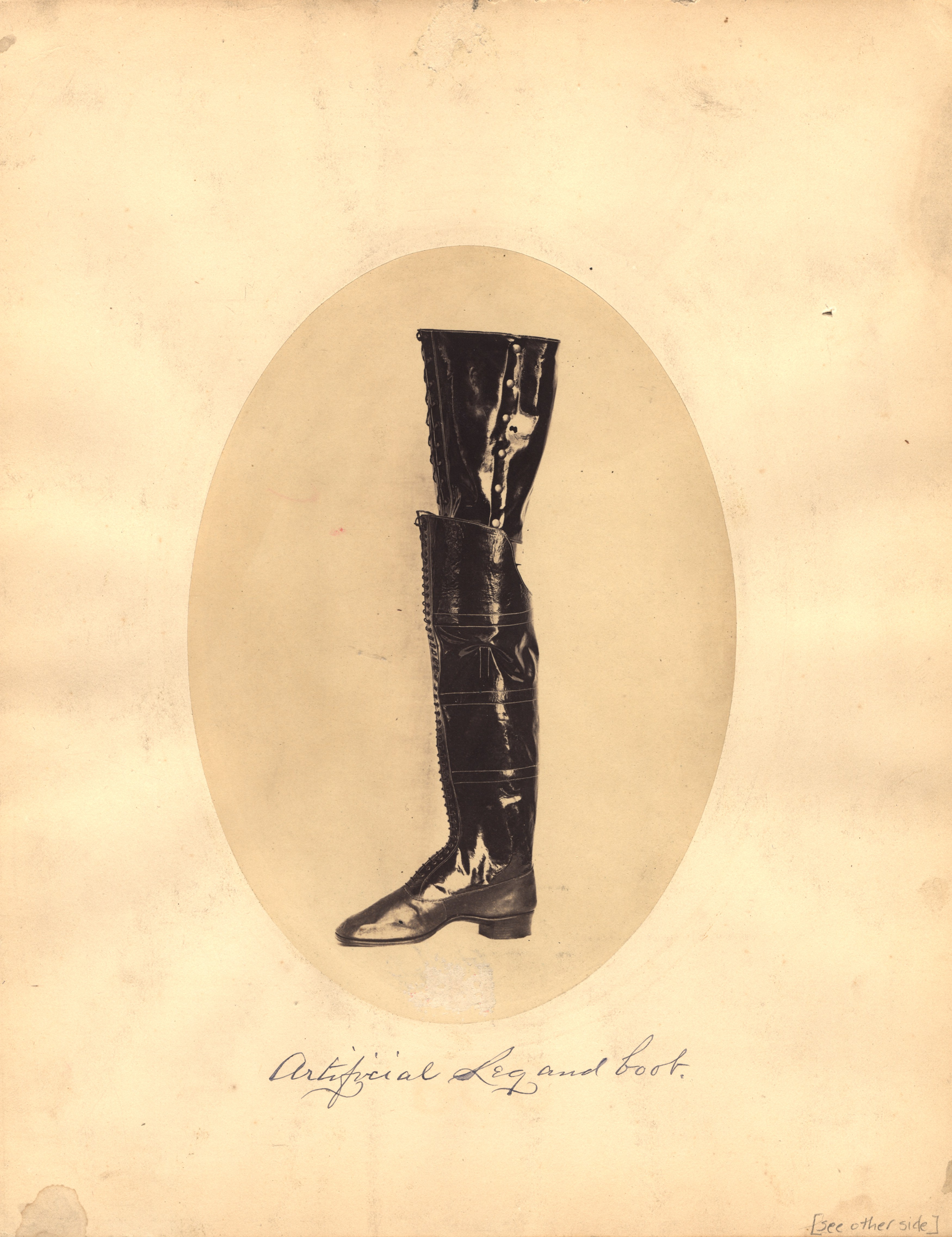
An artificial leg from the American Civil War.
Today, the U.S. Department of Veterans Affairs is a major provider of prosthetics and a leader in rehabilitation treatments for veterans who lose their limbs during their service. These patients are at risk for polytrauma, meaning they have injuries on multiple body parts, usually from blast-related events.
When this happens, these veterans need multifaceted clinical care and a support network. The Rehabilitation Medicine division at the NIH Clinical Center and the National Center for Medical Rehabilitation Research at the Eunice Kennedy Shriver National Institute of Child Health and Human Development help treat prosthetic users and conduct research about limb loss.
Improvements in design
While prosthetics were still made of combinations of wood, metal, glue, and leather even up to the 20th century, they were becoming more functional. From the late 15th century to the 19th century, France and Switzerland were making artificial limbs that could rotate and bend using cables, gears, cranks, and springs. However, these devices still needed to be adjusted manually. For example, an artificial hand could be cranked shut around a fork, but the person still needed another hand to operate the crank.
During the 1900s, manufacturers started to build more functional prosthetics by swapping wood and leather for plastics and other artificial materials. Still, some of the best prosthetics were out of reach for most people, including veterans. Many of these devices were only designed for specific tasks such as piano playing. They would not become more accessible to veterans until World War I, when prosthetic manufacturing for soldiers with limb loss increased in Great Britain. According to Jeffrey S. Reznick, Ph.D., Chief of the National Library of Medicine History of Medicine Division, such wartime manufacturing (and repair) sometimes occurred in military hospitals. Soldiers recovering in those facilities were fitted with artificial limbs as part of their care.
Today’s prosthetics look and work very differently from those made before the late 20th century. More lightweight and durable materials such as plastic, aluminum, titanium, and silicone are common in today’s prosthetic devices. They also fit closer to the user’s remaining limb. The Walter Reed National Military Medical Center will even tattoo service members’ prosthetics to help them look and feel more natural.
But what if a prosthetic could move without the user consciously controlling it? That is what the next generation of artificial limb technology aims to do.

An example of a modern bionic prosthetic arm.
NIH-supported innovations in prosthetics
Scientists are developing robotics, 3D printing, artificial intelligence, virtual reality, and motion-sensing technologies for prosthetics. Over the last decade, NIH has funded several projects that harness the brain’s electrical activity to move prosthetic limbs using electrodes implanted in a person’s remaining muscles. These electrodes send signals to the brain and allow the prosthetic limbs to move more freely.
One example of research funded by the National Institute of Biomedical Imaging and Bioengineering is a robotic lower leg prosthesis that creates a more natural walking motion. Researchers at Vanderbilt University created the device with powered knee and ankle joints and with software that can anticipate how the user wants to move.
In addition to these technological advances, it’s also important to track how many people use prosthetics and what treatments work best for these patients. That’s why NIH, together with the U.S. Department of Defense and the Mayo Clinic, helped create the Limb Loss and Preservation Registry in 2020. This registry uses electronic health records to measure how many people in the United States have limb loss and understand the costs and treatment outcomes for these patients.







