What is lymphedema?
Lymphedema is chronic swelling that happens when something upsets the lymphatic system. The lymphatic system is part of the body’s immune system and includes tissues like bone marrow and bowel lining; blood vessels; and organs like your tonsils, spleen, and lymph nodes.
The lymphatic system works to move a clear, watery, protein-rich fluid called lymph into your bloodstream. Lymph contains lymphocytes, or white blood cells, which attack viruses and bacteria when they enter your body. If you’ve ever been sick and felt a swelling or tenderness in your neck or armpits (where some of your major lymph nodes are), you’ve felt your lymphatic system at work.
Sometimes, though, the lymphatic system gets blocked due to obesity, serious injuries, or genetic problems. When this happens, lymph draining from body tissues has nowhere to go and gets stuck in the tissue. When enough lymph builds up, you swell up. This swelling can negatively affect your quality of life.
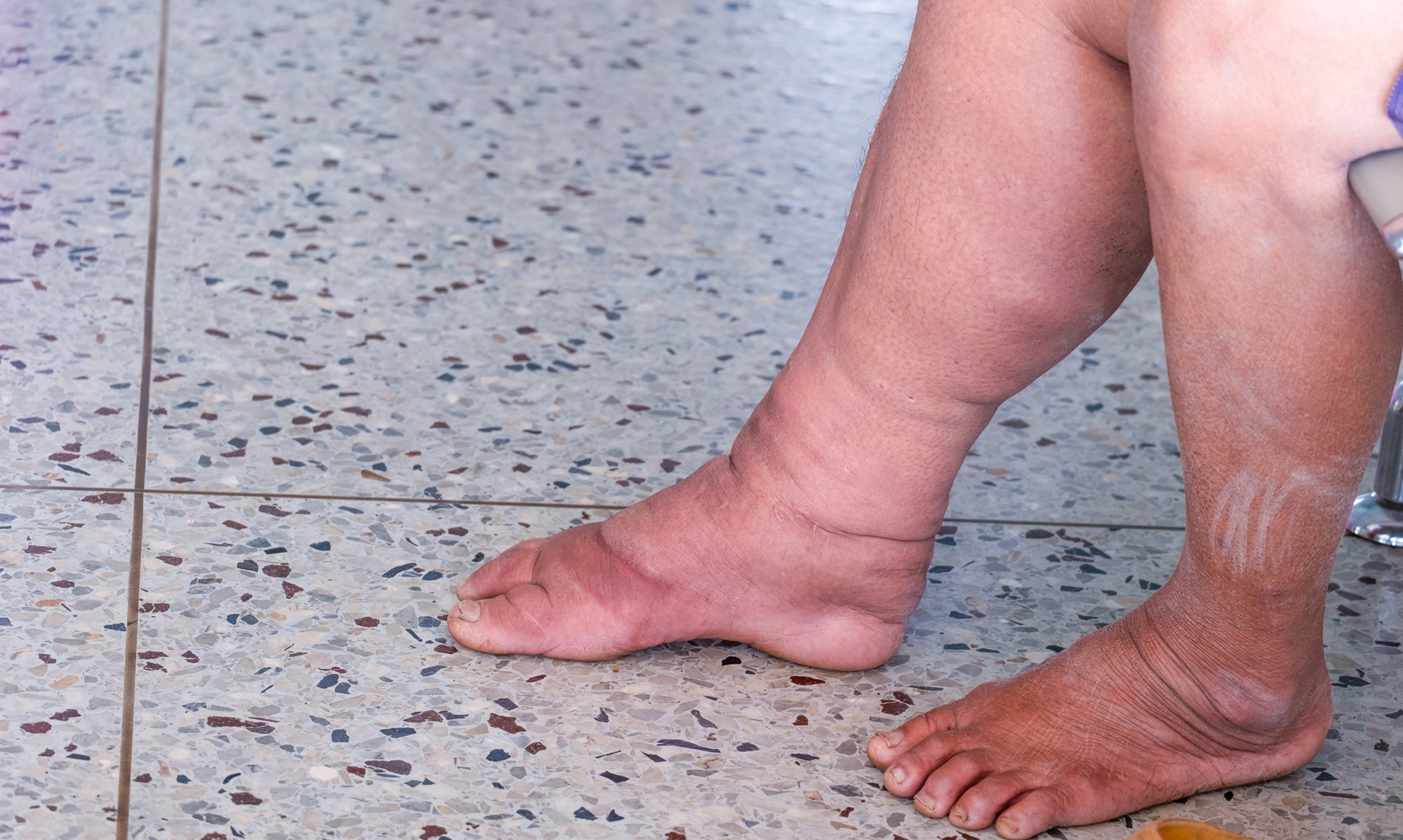
What does that swelling look and feel like?
Lymphedema swelling typically occurs in the arms or legs. Symptoms can include:
- An arm or leg feeling heavy or full
- Skin in the swollen area feeling tight
- Difficulty moving a joint in the arm or leg, including those in the hands and feet
- Skin becoming thicker
- Itching in the legs or toes
- A burning feeling in the legs
How is it diagnosed?
Many things, like infection or blood clots, can cause swelling in the limbs. Only a medical provider can give an official lymphedema diagnosis. When a medical provider looks at a swollen limb to see if it's lymphedema, they might do the following to rule out other possibilities:
- A physical exam and medical history. A medical provider might measure your swollen limb to compare it to the other limb; look for lumps or other signs of disease; and ask about your health habits, past illnesses, and treatments.
- Lymphoscintigraphy. A medical provider will inject a small amount of radioactive substance into the body and observe how it flows through the lymph nodes.
- Magnetic resonance imaging (MRI). A medical provider will use a magnet, radio waves, and a computer to take detailed pictures of areas inside the body.
- Indocyanine green (ICG) lymphography. A medical provider will inject a small amount of ICG—a medical dye used for diagnostic imaging—into the body and observe how it flows through the lymphatic system.
How is it treated?
Some early stages of lymphedema can go away without treatment. There is no cure for later stages of the condition—once the lymph system is damaged, it cannot be repaired. However, that does not mean that lymphedema symptoms can’t be managed. A medical provider might suggest a plan that includes:
- Weight loss and exercise to help lymphatic vessels move trapped lymph fluid.
- Compression of the area through things like special physical therapy or compression garments to help move lymph fluid and keep it from building up in your body.
- Physical therapy like special massage and skin care to help reduce swelling and protect the skin.
- Some newer treatment options like lasers and stem cells, which have been shown in small studies to be an effective treatment for lymphedema.
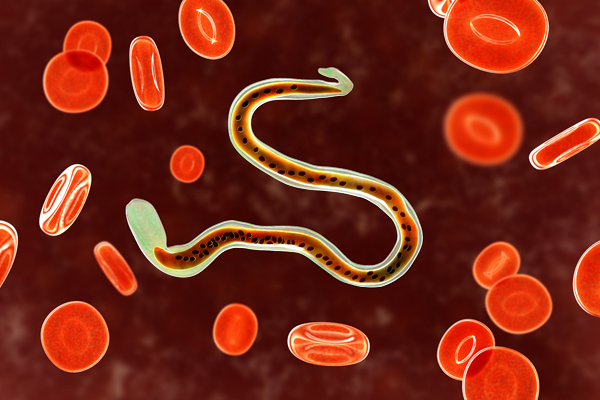
Wuchereria bancrofti, the causative agent of lymphatic filariasis.
Who is at risk for lymphedema?
There are two types of lymphedema:
- Primary lymphedema occurs when the lymphatic system doesn’t develop properly and is extremely rare, affecting roughly 1 out of every 8,000 individuals worldwide.
- Secondary lymphedema occurs when the lymphatic system is damaged by something else, often through cancer treatment or parasite infections, and is the most common type of lymphedema. Roughly 1 in 1,000 Americans have secondary lymphedema, and it’s believed to affect as many as 140 million to 250 million people worldwide.
Secondary lymphedema is often associated with cancer and cancer treatment. Tumors that press against lymph nodes can create blockages, and radiation can affect lymph nodes and create scar tissue that blocks the flow of fluids. Surgery that removes organs or tissues affected by cancer can sometimes remove lymph nodes as well.
NIH research to end lymphatic filariasis
Parasitology is a field of medicine that focuses on the study of parasites—small organisms that survive by living off the human body. The Parasitology and International Programs Branch and the Laboratory of Parasitic Diseases at the National Institute of Allergy and Infectious Diseases (NIAID) are supporting and conducting multiple research projects aimed at treating and ending a kind of lymphedema called lymphatic filariasis. This disease is a form of secondary lymphedema caused by microscopic worms entering the lymph system via an infected mosquito bite.
Lymphatic filariasis affects more than 120 million people in tropical areas across 72 countries and is considered a neglected tropical disease (NTD). Because NTDs generally affect some of the world’s poorest communities, they historically haven’t gotten the same amount of attention or research funding as other diseases. The at-risk population for lymphatic filariasis includes 1.2 billion people worldwide.
NIAID-supported researchers are working to make lymphatic filariasis a problem of the past. Some labs are working to develop better treatments for people who have lymphatic filariasis, and other labs are working on tests to detect the disease and help curb its spread. A vaccine for the disease is currently in early stages of development.